The FDA has approved the first digital pill
05/04/2018 / By Isabelle Z.

It’s every thinking person’s worst nightmare: A digital pill. The prospect of ingesting risky pharmaceuticals combined with tracking microchips that transmit biological data from your body might sound like something we won’t need to worry about for a long time, but the truth is that this technology is already here, and the FDA has even given it its stamp of approval.
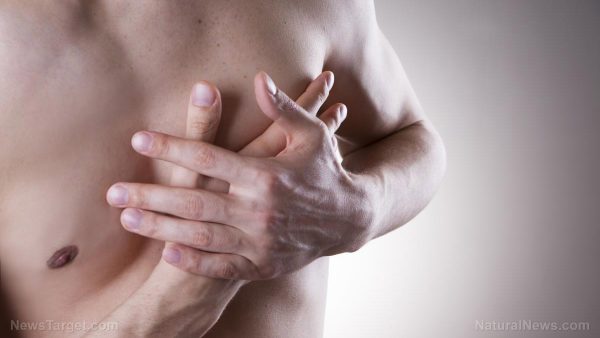
The medication has a sensor embedded inside of it that will tell doctors if and when patients take their medication. About the size of a grain of sand, it contains magnesium, silicon and copper, and it creates an electric signal when it comes into contact with stomach fluid. In other words, the patient basically serves as the battery.
The patient must also wear a patch that is not unlike a bandage on their left rib cage; the patch must be changed once a week. This patch sends the patient’s activity level and the date and time they took the pill using Bluetooth and a cell phone app. Patients can also add their mood and other information to the app, which is then transmitted to a database for physicians to access. The pill allegedly only works for around three minutes.
The first digital pill is a version of the antipsychotic drug Abilify, which is a very curious choice. The drug, whose generic name is aripiprazole, is given to people who have bipolar disorder, major depressive disorder, or schizophrenia. In other words, this technology, which is enough to induce paranoia in even the most stable individuals, is being given to people with illnesses associated with paranoia and delusions. What could possibly go wrong?
Dr. Paul Appelbaum of Columbia University’s Psychiatry Department told the New York Times that one of the reasons these patients don’t take their medications regularly is out of paranoia about their doctor or their doctor’s intentions.
“A system that will monitor their behavior and send signals out of their body and notify their doctor?” he asked. “You would think that, whether in psychiatry or general medicine, drugs for almost any other condition would be a better place to start than a drug for schizophrenia.”
Bad for people, but good for profits
Does anybody really want this? In short, yes; pharmaceutical companies want this very much, and so do doctors. According to a report published in Pharma Marketing News, an 18 percent increase in medication compliance could lead to increased revenue for health care services and doctors of around $8,000 per patient every year!
They justify this not by pointing out all the profits they stand to gain but by frightening patients into thinking of what could happen if they don’t take their meds for whatever reason. It is believed that half of all patients do not follow the instructions for taking a proper dosage of the medication they are prescribed. Therefore, they caution that failure to take a prescribed course of medication could make a person’s symptoms get worse and see them end up hospitalized. In other words, those kind pharmaceutical companies just want to help you remember to take your pills because they care about your well-being so much.
That’s funny considering the medication has only been approved so far for tracking doses; it hasn’t yet been proven to improve a patient’s adherence.
Another interested party in this unsettling technology is insurers, who could eventually offer patients incentives to use the pills because they can keep their costs down. Indeed, some experts worry that digital pills could become so incentivized by insurance companies that patients essentially feel coerced into taking them, which raises even more ethical questions.
This “biomedical Big Brother,” as Columbia University Chairman Dr. Jeffrey Lieberman termed it, is an incredibly unsettling concept, and you don’t need a mental disorder to feel paranoid about where all this is headed.
Sources for this article include:
Tagged Under: Abilify, Big Brother, Big Pharma, digital pills, disease treatments, Microchips, paranoia, privacy watch, schizophrenia, sensors, surveillance, tracking